Why staying home during a pandemic can increase risk for some
By Dr Katrina Raynor, Dr Ilan Wiesel, Professor Bec Bentley
Affordable Housing Hallmark Research Initiative
As coronavirus infections began to rise in Australia, citizens were ordered by government to stay home. “If you can stay at home, you must stay at home” has become the motto for good citizenship, and our primary weapon against a cureless pandemic. However, over less than two months, the experience of staying home exposed the inadequacy of housing for many people.
As coronavirus infections began to rise in Australia, citizens were ordered by government to stay home. “If you can stay at home, you must stay at home” has become the motto for good citizenship, and our primary weapon against a cureless pandemic. However, over less than two months, the experience of staying home exposed the inadequacy of housing for many people.
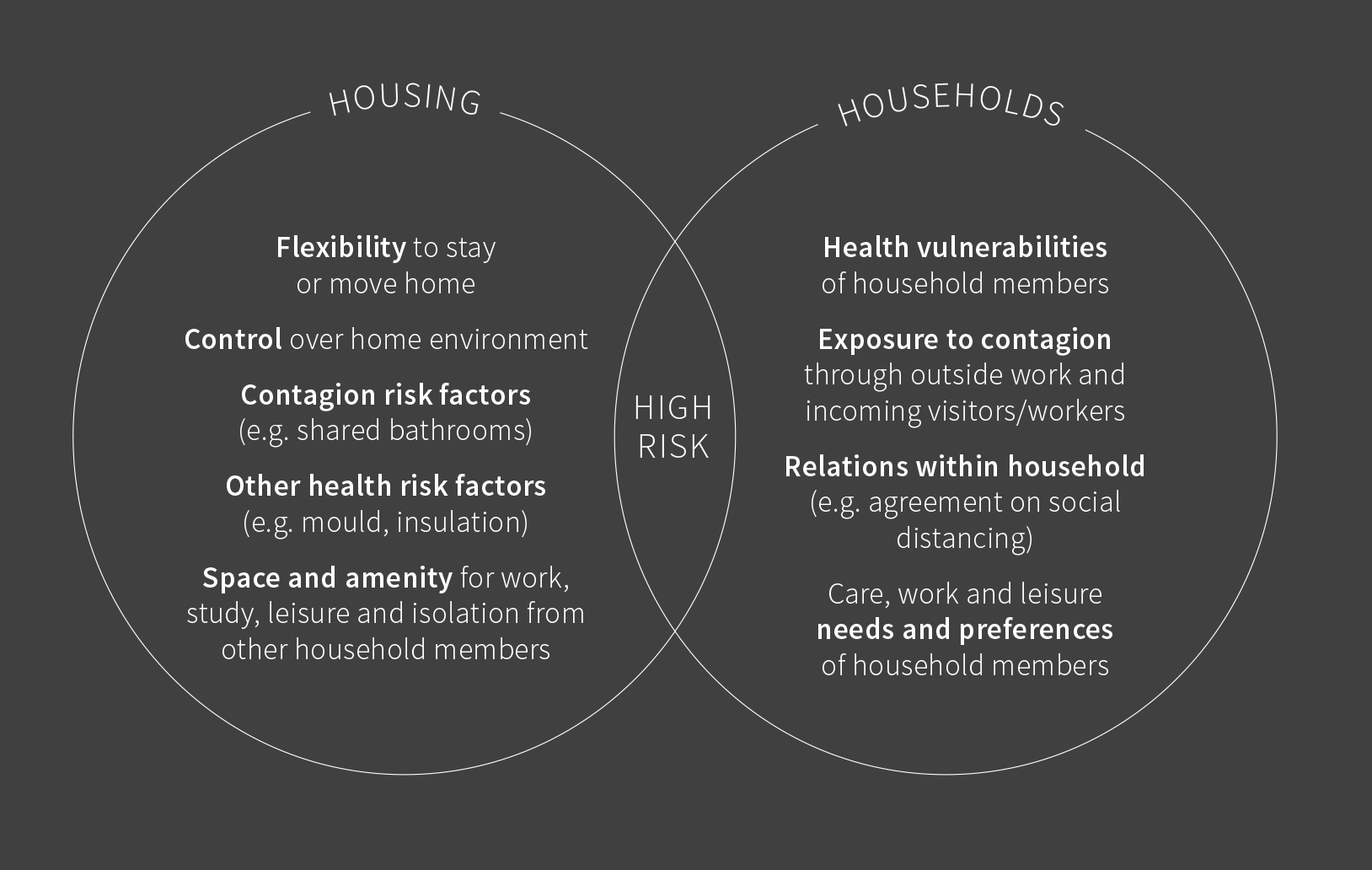
Housing features such as tenure, density and design have become key factors determining people’s ability to stay home, to work or study from home effectively, to isolate from other members of the household if necessary, and more generally to protect themselves and others, especially those who are more vulnerable, from the risk of contracting coronavirus.
Housing tenure, design and quality influence ability to stay home
Security of tenure, capacity to adapt to changing circumstances and affordability all play a role in resident’s ability to shelter safely during COVID19. Even before COVID19, over two-thirds of low-income renters in Australia were in housing stress and over 31% of renters were in leases of 6 months or less. With limited ability to make changes to their homes or ask for repairs tenants also have less capacity to adjust their homes to allow for safe segregation of occupants if necessary. Confronted with high levels of insecurity and low affordability, renters may move to overcrowded homes to share housing costs or find themselves homeless or couch surfing; both movements are associated with higher risks of contagion. Many households may unexpectedly find themselves in this situation due to the economic downturn triggered by COVID. Such conditions are amplified for international students who cannot return home, may have lost casual work and face uncertainty in the short to medium term about their housing.
Homeowners face other restrictions in their ability to stay home. Homeowners have far less flexibility to move if they find their home is inappropriate for safe isolation. There is growing evidence that many households are forming and dissolving in response to COVID19 job losses and shelter-in-place measures. Younger people are moving home to their families, international students have returned to their countries of origin (or didn’t come to Australia in the first place) and many households have relocated as they no longer require proximity to their work places. Such movements are much easier for renters that face lower transaction costs when moving.
The physical design of homes is a critical factor shaping their capacity to provide safe shelter. This may be seen in overcrowding of homes that reduce capacity to isolate from other residents. As clusters of COVID19 linked to overcrowded dormitories in Singapore have shown, internal densities and extended close contact in indoor spaces are key factors in the spread of COVID-19. It is not density itself that is necessarily the problem but the ways homes are designed to manage different densities. Places that promote sustained contact while indoors, like dormitories, rooming houses or hospitals, present far higher risks of contagion. This will also be a consideration in apartment lobbies and lifts.
The impact of buildings also manifests in differing levels of housing quality and amenity – isolating in drafty, poorly-insulated and mouldy homes only serves to exacerbate health concerns. Similarly, households now balancing work, leisure, home-schooling and domestic activities all in one space will know well the fine balancing act of juggling multiple uses in one space. Small homes and those designed without children in mind will be particularly challenging at this time. Confinement, loss of routine and reduced contact causes stress, as well as boredom, frustration, and sense of isolation. As we turn to new or existing hobbies such as baking, gardening, exercising or craft projects, some homes will have space for these activities while many others do not.
Risks and resources are shared between household members staying home together
The pandemic has highlighted the interdependency between members of the household, and inequalities between different types of households. The composition of a household - the profile of occupants, their combined resources and relationships to one another - determines occupants’ capacity to ‘stay safe and stay home’. It is not enough to consider the health risk factors of an individual without reference to their household. For example, all members of a household need to take extra precautions when staying home with an elderly or immuno-compromised occupant.
People living in share houses face a unique profile of challenges. Household members may not hold the same views on compliance with government recommendations. People have reported concern about housemates having visitors or working in the health care sector. Where one member of a share house moves out, there are potential repercussions for remaining members’ rent and their ability to sustain their tenancy.
Working and studying from home has also presented challenges for share households. Simple examples include sharing internet connections during peak time and finding space in the house for each household member to work or study effectively. Further to this, some households report a lack of control over internet plans and infrastructure upgrades that will enable them to work and study online.
All household members share exposure in a pandemic. If one household member is an essential or key worker who needs to continue to travel and be in contact with others in the community, all household members’ risk is higher. This has been demonstrated by the recent outbreak of COVID cases centered around Cedar Meats in Victoria whereby family of employees of the meat processing plant were amongst those infected. It is also why the provision of temporary housing for healthcare workers who need to shelter away from their households was such a wise move.
During the COVID-19 pandemic, the interdependency and shared risk within households has been exposed in its most extreme in congregate residential facilities. Aged care homes, in particular, have emerged as the epicentre of contagion and death in the coronavirus pandemic.
In some of the worse affected countries, such as the United States, Belgium and Sweden, it is estimated that between a third and a half of all COVID-19 deaths occurred in aged care facilities.
In Australia approximately one in three deaths occurred in aged care facilities. The susceptibility of aged care facilities results from a combination of factors including: a high concentration of people with underlying health risk factors; exposure to other residents in common facilities, often including kitchens and bathrooms; and exposure to infection through staff and visitors moving in and out of the facility and in direct physical contact with residents. A similar suite of concerns are relevant for people with disability who require support workers and family to visit their home. People with disabilities have less capacity than other community members to minimise and regulate their exposure, causing concern for themselves, their families and advocates.
Attempts to protect aged-care residents from infection have included strict social distancing measures, including controversial bans on visitors, which left many residents socially isolated and reduced community monitoring of the standard of care provided in these facilities.
216,000 residential aged care places have been provided in Australia in 2018. In addition to these, other forms of congregate facilities – such as supported housing, large residential institutions for people with intellectual disability, and prisons – share similar vulnerabilities.
Housing matters now more than ever
Lockdown restrictions are now easing in Victoria and the ‘stay home’ directive was formally replaced with a ‘stay safe’ message on 1st June. However, until a cure or vaccination is made available en masse, COVID-19 is here to stay, with the possibility of new restrictions reinstated whenever infections rise above a predetermined threshold.
The way we think about health, housing, risk and vulnerability needs to change to reflect the ‘new normal’ of increasingly frequent viral pandemics. Housing and household risk are overlapping concepts and policy responses can’t afford to consider these ideas in silos. Access to secure and affordable housing plays a substantial role in public health and safety during a pandemic, just as considering the composition of households can extend traditional thinking about individual health risk factors.
Housing inequalities have always compounded and reflected inequalities in health, wellbeing, and productivity. The imperative to stay home during COVID-19 has amplified these effects. Alongside individual characteristics such as poor health, low income, age and gender, housing related factors are now significant factors mediating vulnerability to, and the varied experiences of, the COVID-19 pandemic. The way that people are housed matters more than ever and the consequences for people’s health (including their mental health) and economic security are greater than they have been in most of our lifetimes.
Dr Katrina Raynor, Dr Ilan Wiesel, Professor Bec Bentley.
Dr Katrina Raynor, Faculty of Architecture Building and Planning, katrina.raynor@unimelb.edu.au
Dr Ilan Wiesel, School of Geography, ilan.wiesel@unimelb.edu.au
Professor Bec Bentley, Melbourne School of Population and Global Health, brj@unimelb.edu.au
The Hallmark Research Initiative for Affordable Housing is researching the ways in which housing has cushioned or amplified experiences of vulnerability or resilience during COVID19.
To join the discussion or find out more, contact affordable-housing@unimelb.edu.au.